Conditions we treat


Conditions We Treat
Bentham Physiotherapy Clinic treats many different musculoskeletal conditions including:
- Back Pain
- Disc Prolapse
- Sciatica
- Whiplash
- Neck Pain
- Cervical Headaches
- Frozen shoulder
- Rotator cuff problems
- Osteoarthritis
- Knee Injuries
- Sports injuries
- Tendonitis
 Back Pain
Back Pain
Back pain occurs in 80% of people at some time in their lives, sometimes becoming a recurrent problem. It is not normally due to any serious disease but it can cause acute pain and you may need to reduce the provoking activities for a time. Simple pain medication can also help in the early days which your GP can advise on. We now think that resting for too long (more than a couple of days) usually does not help and may do more harm than good. Your back is designed to move and getting back to normal activities as soon as the pain allows will get you back to normal as soon as possible.
Most back pain comes from the muscles, ligaments and joints of your back, if an Xray is requested, findings most often are normal for age, indicating that the spine itself is not damaged.
Your physiotherapist can give valuable advice for acute pain along with gentle treatment possibly including massage, TENS and acupuncture. They will give you exercises and activities to get you back to full fitness as quickly as possible. Most acute back pain will settle within 6 weeks. Chronic Back Pain (>3months) may require active rehabilitation of the muscles and joints of the spine, sometimes they may also benefit from stretching and mobilisation techniques to help. Your physiotherapist will be able to advise the best exercises to do at any one stage and how to progress these over the course of your treatment.
 Disc Prolapse
Disc Prolapse
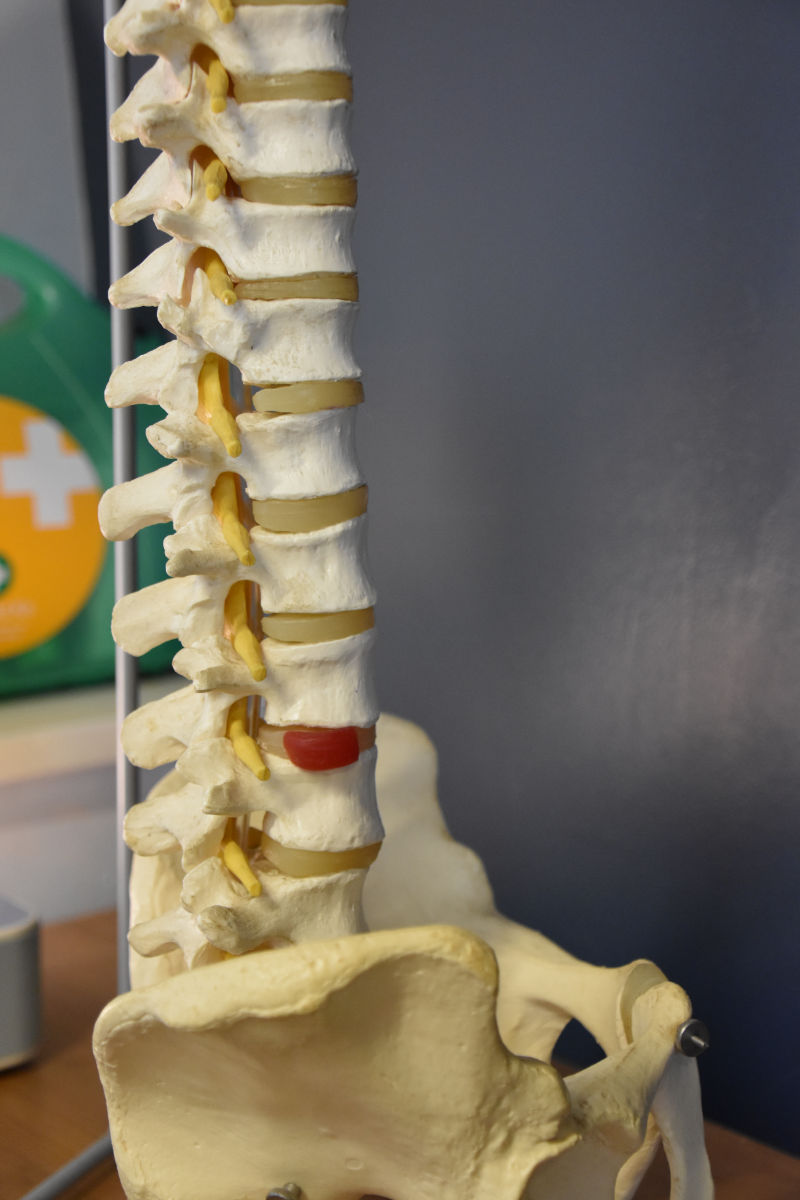
In a few cases of back pain, the fibrous disc between the vertebrae can become inflamed and sometimes protrudes so that it can put pressure on a spinal nerve giving referred pain down the leg and sometimes weakness and pins and needles. This is commonly called a “slipped disc” but in fact the disc has not moved, it protrudes out of its capsule hence the name disc prolapse. Most prolapsed discs will recover with gentle exercise and avoidance of the provoking movements, which in most cases is bending, prolonged or poor sitting posture or lifting. Your physiotherapist will be able to advise on the best exercises and pain relieving treatments, as well as education on prevention for the future.
Sciatica
This is the term for referred pain down the leg. It can come from pressure on spinal nerves, muscular trigger points, tight spinal joints, neural tension and many other causes. Following your assessment your physiotherapist will be able to tell you the most likely cause and offer various treatments to help.
Neck Pain
Neck pain can be due to different conditions including muscle strain, ligament sprain (as in whiplash) or osteoarthritis (often called cervical spondylosis). Following assessment your physiotherapist will be able to advise on the best exercises and treatment techniques to improve your condition.
 Cervical Headaches
Cervical Headaches
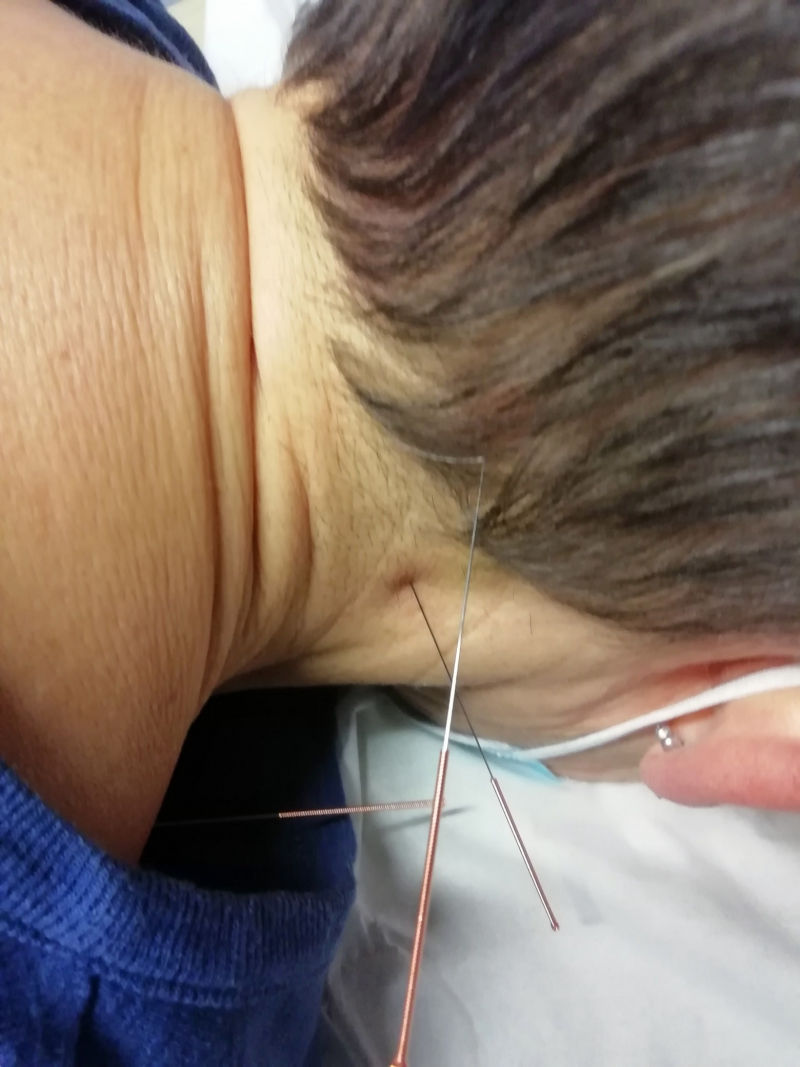
Cervical Headaches are headaches where the cause of the pain is due to tension in the upper neck. Often due to prolonged poor posture, muscle tension, and whiplash type disorders, they can also be affected by stress, poor sleeping position, eyesight disorders and tempero-mandibular dysfunction (jaw).
Your physiotherapist will assess the problem and be able to use different treatment techniques including deep friction therapy, upper cervical strengthening or acupuncture to help alleviate the headaches. Long term, the biggest help can be identifying the trigger to the tension and then working on ways to minimise this e.g. Posture and relaxation strategies, which your physiotherapist can advise on.
Frozen shoulder
Frozen shoulder (sometimes called adhesive capsulitis) is a condition where the shoulder joint capsule stiffens up and can become very painful. Symptoms include pain with movement, pain at night, decreasing shoulder movement over a period of weeks and months. It is thought to be caused by inflammation of the capsule which then leads to adhesions and scar tissue forming. It sometimes occurs following an injury but not always. Without treatment, symptoms usually go but this may take up to 2-3 years. Various physiotherapy treatments including acupuncture, stretching and trigger point therapy may ease pain and improve the movement of the shoulder, your physiotherapist can advise on these. Sometimes a shoulder injection will be necessary to reduce pain, your physiotherapist will liaise with your GP if this is necessary.
 Rotator cuff problems
Rotator cuff problems
The rotator cuff is the group of 6 muscles that blend into the shoulder joint capsule to give the shoulder joint dynamic stability, helping to control the joint during movement. Correct movement patterns around the glenohumeral joint and the scapulohumeral joints are essential for normal, painfree function of the shoulder. Pain and dysfunction can occur with overuse, poor movement patterns or trauma. Initially leading to local impingement pain but if left untreated can sometimes go on to require surgery.
Symptoms often include pain and or weakness on lifting your arm above 90 degrees.
Your physiotherapist will assess your movement and be able to identify abnormal patterns and weakness around the cuff, then teach you the best ways to correct these. Typically your home programme of exercises will be about 12 weeks.
Osteoarthritis
Osteoarthritis is the term given to degeneration of the articular cartilage of any of the joint surfaces of the body. It is often age related and often is due to an injury when younger. It can also be hereditary. Symptoms may include joint pain, tenderness, stiffness, locking, and sometimes swelling and deformity. Often with early osteoarthritis, the pain is due to soft tissue restriction and tenderness, which can respond very well to deep tissue massage, and rehabilitation exercises to strengthen and stretch the affected joint.
 Knee Injuries
Knee Injuries
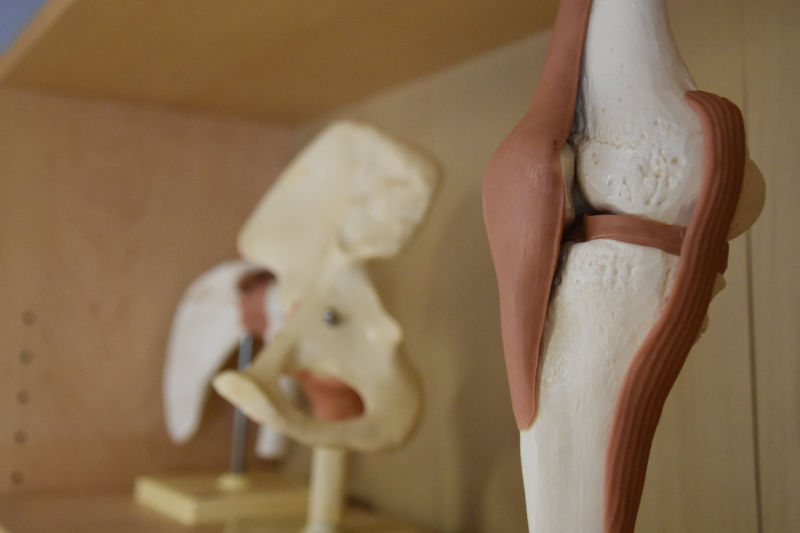
This includes ligament strains or tears, cartilage problems, osteoarthritis in the knee and patello-femoral pain. Each problem will be diagnosed by your physiotherapist using specific tests, and you will be given your home programme to work on along with appropriate treatment in clinic, including deep tissue massage, acupuncture, ultrasound.
 Sports injuries
Sports injuries
Your physiotherapist will be able to assess your acute sports injury and give you a diagnosis and likely prognosis for recovery. Initially treatment will be aimed at relieving swelling and pain, but almost immediately gentle exercise will be advised to ensure your movement and strength are not overly compromised. These will be progressed as you improve. Longer term your physiotherapist will look at any underlying reasons that may have contributed to the injury e.g. old injuries, poor biomechanics, weakness and they will be able to advise on ways to tackle these.
Tendonitis
This includes conditions such as plantar fasciitis, achilles tendonitis, tennis/ golfers elbow, trochanteric pain syndrome. Tendonitis is an acute inflammation of a tendon that often becomes chronic, changing the tendon structure and leaving it weak and not able to tolerate normal loads. Treatment will include strengthening, correction of movement patterns, and biomechanical correction if necessary. Your rehabilitation programme will take at least 12 weeks of home exercises associated with occasional clinic visits to monitor and progress your programme.

